Receiving a long-term disability denial based on a “pre-existing condition” can feel frustrating and unfair. Many claimants are shocked to learn that their insurance company is refusing benefits based on medical treatment that occurred months, or even years, before they stopped working.
If your long-term disability (LTD) claim was denied because of a pre-existing condition, you’re not alone. This is one of the most common reasons insurance companies give for denying benefits.
The frustrating part? These denials are often based on broad interpretations of your medical history—not just what your condition actually is today.
Let’s break this down in plain English.
What Is a “Pre-Existing Condition” (in Simple Terms)?
Most disability insurance policies say a condition is “pre-existing” if you:
- Received treatment
- Took medication
- Saw a doctor
- Or even discussed symptoms
during a certain period before your coverage started (often 3–12 months).
If your disability is later considered related to that condition, the insurance company may deny your claim.
Common Reasons Insurance Companies Deny These Claims
1. You Saw a Doctor Before Your Coverage Started
Even a routine visit can be used against you.
Example: You mentioned back pain once before your coverage began. Years later, you become disabled due to a serious spinal condition. The insurer may argue it’s the same issue.

2. They Say Your Current Condition Is “Related” to Something Older
Insurance companies often connect past and current conditions—even when the link is weak.
Example:
- Prior anxiety → later disability from depression
- Occasional headaches → later chronic migraines
They may treat these as the same condition.
3. They Focus on Symptoms, Not the Diagnosis
You may not have had a diagnosis yet—but insurers argue you had the early signs.
Example: You had fatigue before coverage started, but were later diagnosed with an autoimmune disease. The insurer may say the fatigue was the same condition all along.

4. They Use Any Mention in Your Medical Records
Even a brief note in your records can be used.
Example: A chart note saying “history of back pain” or “complains of fatigue” may be enough for the insurer to deny your claim.

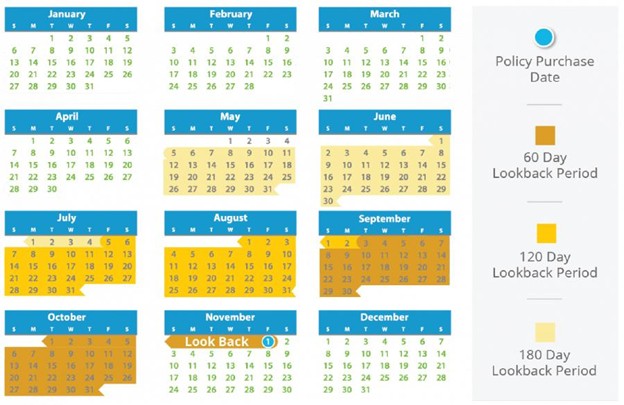
5. They Apply the Rules About Timing Very Strictly
These denials often depend on when things happened.
Most policies look at:
- A lookback period before your coverage started
- A limited time after coverage begins when exclusions apply
If the insurer believes your condition falls within those windows, they may deny the claim.

6. They Rely on Doctors Who Never Examined You
Insurance companies often use reviewing doctors who only read your records.
These doctors may:
- Connect unrelated conditions
- Downplay your treating doctor’s opinion
- Interpret your history in a way that supports denial

The Big Picture
In many cases, the insurance company is trying to:
Link your past medical history to your current disability—even if the connection isn’t strong.
That doesn’t always mean they’re right.
Important: A Denial Is Not the End
Many valid disability claims are initially denied for “pre-existing conditions” and later approved on appeal.
Why?
Because the real issue often comes down to:
- Whether the conditions are truly related
- Whether the insurer is interpreting the policy too broadly
- Whether the medical evidence actually supports their conclusion
When to Get Help
If your claim was denied for a pre-existing condition, it may be worth having it reviewed—especially if:
- Your current condition is different from what you had before
- Your earlier symptoms were minor or unrelated
- The insurance company is stretching your medical history
Bottom line: Just because an insurance company says your condition is “pre-existing” doesn’t mean that decision is final—or correct.
How to Appeal LTD Denials for Pre-Existing Conditions
If your claim was denied based on a “pre-existing condition,” the appeal is your opportunity to tell the full story correctly—with the right medical and legal support.
Here are some of the most effective strategies used to challenge these denials:
1. Focus on the Policy Language (Not Just the Medical Records)
Insurance companies rely on specific wording in the policy—phrases like:
- “caused by”
- “contributed to by”
- “resulting from”
Those words matter.
A key question in many appeals is:
Is your current disability truly caused by the earlier condition—or is the connection being stretched?
A careful reading of the policy often reveals that the insurer is applying the exclusion more broadly than allowed.
2. Separate Past Symptoms from Your Current Condition
One of the most important strategies is showing that:
- Earlier symptoms were not the same as your current condition
- Or were minor, temporary, or unrelated
Example: Occasional back discomfort is not the same as a disabling spinal condition.

Your appeal should clearly explain how your condition changed over time.
3. Build a Strong Medical Narrative from Your Treating Doctors
A detailed statement from your treating doctor can be critical.
It should address:
- When your disabling condition actually began
- Whether it is related to (or different from) earlier issues
- Why prior symptoms do not explain your current limitations
This helps counter the insurance company’s file reviewers who never examined you.
4. Create a Clear Timeline
Many denials fall apart when the timeline is properly laid out.
An effective appeal will show:
- When coverage started
- What happened during the “lookback period”
- When symptoms actually worsened
- When the condition became disabling
This can expose errors in how the insurance company applied the timing rules.
5. Challenge Weak or Overbroad Medical Reviews
Insurance company doctors often:
- Rely only on paper records
- Make assumptions about “related conditions”
- Ignore key evidence
Your appeal can point out:
- Gaps or inconsistencies in their analysis
- Failure to address treating doctor opinions
- Lack of a direct connection between conditions
6. Emphasize the Lack of a Direct Connection
A strong appeal often comes down to this idea:
A past condition must have a clear, direct connection to your current disability—not just a possible or indirect link.
If the insurer is relying on a “maybe” or a loose connection, that can be challenged.

7. Submit All Supporting Evidence During the Appeal
Under most disability policies (especially employer-sponsored plans), the appeal is your best—and sometimes only—chance to fully develop the record.
That means submitting:
- Medical opinions
- Clarifying records
- Personal statements (when helpful)
- Any evidence that addresses the insurer’s reasoning
Waiting until later can limit your options.
The Bottom Line With Appeals
Appealing a pre-existing condition denial is not just about sending more records.
It’s about:
- Framing the medical story correctly
- Applying the policy language carefully
- Challenging assumptions the insurance company made
With the right approach, many of these denials can be successfully overturned.
Other Common Reasons for Long Term Disability Insurance Denials
Navigating insurance claims can be tricky. Understanding why denials occur can help in avoiding them. Insurers often give specific reasons for denials.
One common reason is the insurer’s assertion of insufficient medical evidence. They might claim your condition does not meet their definition of disability. Ensuring your medical records clearly reflect your condition is vital.
Another frequent reason involves missed deadlines. Insurance companies have strict timelines for submitting claims and appeals. Missing these can result in claim denials, regardless of validity. Keeping a detailed calendar helps prevent these errors.
In addition, many claims face denial due to lack of documentation. A strong disability claim includes comprehensive records. These should include everything from diagnosis to ongoing treatment evidence.
Common denial reasons include:
- Insufficient medical evidence
- Missed submission deadlines
- Incomplete documentation
- Non-compliance with treatment plans
Understanding these common reasons empowers you. You’ll know where to focus your efforts when submitting your claim.
Gathering Evidence: Medical Records and Documentation
Gathering strong evidence is crucial for your appeal. Start with comprehensive medical records that affirm your condition. They are the backbone of your case, making it vital they clearly support your claim.
Consult your healthcare provider for a detailed medical report. Ensure the report highlights how your condition impairs your ability to work. A well-documented report aligns with the definitions in your policy.
Include any relevant test results and treatments. These can strengthen your case by demonstrating ongoing management of your condition. Consistency in your medical history is key.
Ensure your documentation covers:
- Doctor’s reports and notes
- Test results and medical imaging
- Treatment plans and follow-up visits
Inconsistencies or gaps can harm your appeal. Always double-check for completeness and clarity. Solid documentation provides a strong basis for contesting the denial.
The Insurance Appeal Process: Step-by-Step Guide
Navigating the insurance appeal process can seem daunting. However, with the right steps, you can tackle it more effectively. First, understand the specific reasons for your claim denial. Scrutinizing the denial letter is the starting point.
Next, request a complete copy of your claim file from the insurer. This includes all the evidence they used against your claim. It’s essential to know what you’re dealing with before proceeding.
Develop a strategic appeal letter addressing all denial reasons. This letter should explain why the reasons cited don’t apply to your case. Be concise but thorough in explaining your standpoint.
Follow the insurance company’s appeal procedures carefully. Adhering to their guidelines ensures your appeal is processed correctly. Missing a step can lead to unnecessary delays or outright rejection.
Consider these steps to streamline the process:
- Identify denial reasons
- Request and review your claim file
- Draft a clear appeal letter
- Comply with appeal guidelines
Finally, maintain meticulous records of all correspondences. Keeping track of communication can be invaluable if further disputes arise. Be persistent and patient throughout this process. Despite its complexity, a comprehensive approach maximizes your chance for a favorable outcome.
RELATED POST: How Long Does a Long-Term Disability Appeal Take?
Writing an Effective Appeal Letter
Crafting a persuasive appeal letter is crucial. Start by clearly stating your personal details and policy number. This ensures the insurer can quickly locate your file.
Focus on addressing every denial reason explicitly. Use evidence from your medical records or new documentation to refute their points. Be factual and concise to strengthen your argument.
Present any missed or overlooked information. Highlight discrepancies in the denial letter to cast doubt on the insurer’s decision. A well-organized letter boosts your credibility.
Consider these key elements for your appeal letter:
- Personal and policy details
- Direct refutation of denial reasons
- Presentation of overlooked evidence
- Identification of inaccuracies in denial
Conclude by reiterating your eligibility for the claim. Request a formal review based on the evidence you’ve provided. A well-structured letter can greatly improve the outcome of your appeal.
Addressing Errors and Discrepancies in the Denial Letter
It’s crucial to meticulously review the denial letter for errors. Even small inaccuracies can impact the outcome of your appeal.
Document any discrepancies you discover. Highlight these in your appeal to challenge the insurer’s basis for denial effectively.
Key areas to watch for include:
- Incorrect or missing medical details
- Inaccurate policy information
- Misinterpretation of your condition
Point out these issues clearly in your communication. Request rectification and a re-evaluation of your claim to ensure fairness. Addressing errors promptly can tilt the decision in your favor.
Working with Medical and Legal Professionals
Enlisting the help of medical professionals is vital to support your appeal. They can provide detailed reports that substantiate your claim. Ensure that your healthcare provider clearly outlines how your condition affects your ability to work.
Legal assistance can also play a pivotal role in your appeal. A disability insurance attorney understands the nuances of policy language and can navigate complex legal terrain. They can help draft an effective appeal and negotiate with the insurance company on your behalf.
When working with professionals, make sure they:
- Understand your insurance policy terms
- Have access to all relevant medical records
- Are experienced in disability claims
Collaborating with medical and legal experts strengthens your case. Their expertise could significantly boost your chances of a favorable outcome, offering support through the appeal process.
Navigating Deadlines and Timelines
Understanding the timeframe for your appeal is crucial. Missed deadlines can jeopardize your chances of success. Each policy has specific deadlines, and it’s important to be aware of these.
Create a plan to track critical dates:
- Note the appeal deadline in your calendar
- Set reminders for key dates and tasks
- Review any updates on timelines regularly
Being organized helps maintain your focus. It ensures you meet all necessary timelines during the appeal process, keeping your claim in good standing.
Presenting New Evidence and Strengthening Your Case
Presenting new evidence is vital when appealing a denial. It can tip the scales in your favor. Ensure all new information is relevant to your condition and addresses the denial’s reasons.
Compile any additional documents that demonstrate your current health status:
- Updated medical reports
- Test results showing condition changes
- Statements from healthcare providers
Craft a compelling case by highlighting this new evidence. Clearly explain how it impacts your ability to work. This approach strengthens your appeal by providing a more complete view of your situation.
Understanding Your Rights: ERISA and State Laws
Knowing your rights enhances your appeal strategy. The Employee Retirement Income Security Act (ERISA) governs many employer-sponsored disability plans. Familiarize yourself with ERISA protections to understand legal entitlements.
State laws can also affect claims, offering additional rights and regulations. Be sure to research specific state mandates that might impact your claim.
Here’s a checklist to ensure you know your rights:
- Review ERISA provisions
- Investigate state disability laws
- Consult with a legal expert if needed
These steps ensure you’re well-informed and prepared in your appeal journey.
RELATED POST: What Are Your Legal Rights Concerning Your Claim for LTD Benefits?
What to Do If Your Appeal Is Denied Again
Facing another denial can feel discouraging. Yet, options remain. Persistence is key, even after multiple setbacks.
Here’s what to consider next:
- Consult a lawyer for further advice
- Evaluate alternative legal actions
- Reassess medical documentation for gaps
A denied appeal isn’t the end of the road. In some cases, you may have the option of filing a second, optional appeal. If you have exhausted your appeal options, the next step is filing a lawsuit. Understanding all available paths ensures you make informed decisions going forward.
Tips for Communicating with Your Insurance Company
Effective communication with your insurer can influence the outcome of your claim. Approach each interaction thoughtfully and carefully.
Consider these communication tips:
- Stay calm and professional in every conversation
- Keep records of all interactions and communications
- Prepare key points before calling or writing
Remember, your tone and clarity matter. Being organized and respectful can pave the way for more productive dialogues. If misunderstandings occur, clarify immediately to avoid complications later. Persistence, paired with patience, often yields better results.
Protecting Your Financial and Emotional Wellbeing
Facing a disability insurance denial can be challenging. Maintaining financial and emotional stability during this period is crucial for your long-term wellbeing.
Consider these strategies:
- Establish a budget to manage expenses
- Seek support from family and friends
- Explore counseling for emotional support
A comprehensive plan ensures you’re prepared for uncertainty. Emotional resilience and financial planning work hand in hand, helping you navigate this tough time. Connecting with supportive networks can also offer relief and guidance, which can be invaluable.
Frequently Asked Questions About Pre-Existing Condition LTD Denials
What is considered a pre-existing condition in a long-term disability policy?
A pre-existing condition is typically defined as any illness, injury, or medical condition for which you received treatment, care, medication, or consultation during a specified “look-back” period before your coverage began. This look-back period is often three to 12 months, depending on the policy. Each policy defines pre-existing conditions differently, so it is critical to review the exact language in your plan.
How do insurance companies decide whether to deny a claim based on a pre-existing condition?
Insurers review your medical records to determine whether you received treatment or reported symptoms related to your disabling condition during the look-back period. They may also look for related or similar conditions and argue that your current disability is connected to earlier treatment. In many cases, denials are based on broad interpretations of medical history rather than clear evidence.
Can a long-term disability denial for a pre-existing condition be appealed?
Yes. Most denied claims can be appealed, and many pre-existing condition denials can be challenged with stronger medical evidence and a detailed review of the policy language. The appeal process allows you to submit additional documentation, clarify your medical timeline, and address the insurance company’s reasoning. It is important to carefully review your denial letter and follow all deadlines.
What role does ERISA or state law play in a pre-existing condition denial?
If your coverage is through an employer-sponsored plan, your claim is likely governed by ERISA, a federal law that sets strict rules for the appeal process and deadlines. Individual disability policies may be governed by state law instead. The applicable law can affect your rights, the evidence you can submit, and your options if the appeal is unsuccessful.
What should I do after receiving a pre-existing condition denial?
Start by reviewing your denial letter and your policy’s pre-existing condition language. Obtain and review the medical records the insurance company relied upon, and work with your doctors to clarify your medical history and current limitations. Being proactive and organized during the appeal process can significantly improve your chances of overturning the denial.
Staying Persistent and Proactive
Persistence is key when facing a long term disability insurance denial. Navigating the appeal process requires patience and a proactive approach. Stay informed and don’t hesitate to seek professional guidance.
Remember, every step you take brings you closer to a resolution. Keep detailed records and continuously update your documentation. Your persistence can make a significant difference, turning a denial into an approved claim. Stay positive and advocate for your rights with determination.
If your long-term disability claim has been denied due to a pre-existing condition, Ortiz Law Firm may be able to help. We focus on long-term disability appeals and lawsuits and assist claimants nationwide.
Call (888) 321-8131 or contact us for a free case evaluation to learn about your options and how we may be able to help you challenge the denial and pursue the benefits you deserve.